The recent outbreak of measles has triggered a number of questions about vaccination, public health, and herd immunity. As I have fielded questions from patients, family, and friends about vaccination, I have come to realize this is an area ripe for a bit more detailed discussion.
What are the benefits of immunization? At first glance this seems like an obvious question, but it is more complex than many realize. Depending on the shot, it may provide one or more benefits.
Let’s review why we vaccinate.

IM Vaccination, 1977.
CDC Public Health Image Library.
Common domain.
1st: Vaccination prevents illness in the vaccinated. I think this is the most obvious purpose of vaccination and what most people assume when we talk about the benefits of vaccination.
Example: You don’t want to get tetanus so you get vaccinated for tetanus.
Tetanus (commonly called lockjaw) is caused by a ubiquitous pathogen, Clostridium tetani, that is found in soil and on rusty nails. It sits in wait to be inoculated into your foot when you step on the nail. OK, so that’s the image that tetanus usually conjures, but one can get it from any contaminated wound.
Tetanus is not transmitted person-to-person. If you elect not to vaccinate yourself or your child against tetanus, the only person put at risk is yourself or your child. I would still argue that would be a poor medical decision. Tetanus is a horrific disease, but you would not be putting others at risk by your personal decision.

Vaccination.
CDC Public Health Image Library.
Common domain.
2nd: Vaccination serves to reduce severity of the illness in the vaccinated. In this case, the purpose of vaccination is not necessarily to prevent the infection, but rather to blunt the severity of the infection. This occurs with a number of vaccinations.
Example: Even though a child vaccinated against measles has a small chance of still getting measles, the course of illness and severity of symptoms are reduced.
This is a benefit – anyone would want a milder rather than a more severe illness. And this is commonly seen with a number of vaccinations.

Administration of the oral polio vaccine, 1977.
CDC Public Health Image Library.
Common domain.
3rd: Vaccination serves to reduce complications of the illness in the vaccinated. In this case you may still get the infection, but the risk of specific complications are reduced. I want to emphasize the subtle difference between benefit #2 and #3, by again using the measles example.
Example: You don’t want sclerosing subacute panencephalitis, so you get the measles vaccine.
Sclerosing subacute panencephalitis (SSPE) is a rare neurologic complication of measles occurring an average of 7- 10 (though as late as 27) years after initial infection. SSPE symptoms are progressive and include behavioral changes, cognitive deterioration, neurologic deficits, and ultimately, death. Based on the 1989-1991 epidemic of measles in the United States, researchers calculated an estimate of the risk of SSPE of 22 cases per 100,000 cases of measles. Vaccination prevents SSPE.

Vaccination.
CDC Public Health Image Library.
Common domain.
4th: Vaccination serves to reduce transmission of the infectious disease. This is different than herd immunity (see #5 below), here the vaccine results in decreased shedding of infectious virus or bacteria in the infected. Because fewer infectious ‘germs’ are shed there are fewer secondary infections.
Example: You know you don’t want your family to get rotavirus so you vaccinate your new baby.
Infant vaccination for rotavirus was implemented in 2006 and, not surprisingly, the rate of severe gastroenteritis in the targeted age demographic plummeted. Remarkably though, gastroenteritis rates also fell in kids older than 5 as well as adults. This suggests a reduction in rotavirus infections originating with neonates that spread to older children (siblings) and adults (parents). This larger impact of rotavirus vaccination was a pleasant added benefit.
Parenthetically, I would also note that part of the reason we treat infections is not only to alleviate symptoms and cure the patient, but also to prevent transmission to others. In this case we are using antibiotics or antivirals rather than immunization. Examples include the use of oseltamivir for influenza, antiretroviral therapy for HIV, and azithromycin for pertussis (whooping cough). In all three cases, the treatment has the effect of reducing likelihood of transmission of infection. In the latter case (pertussis), the use of azithromycin is solely to prevent transmission. We treat with antibiotics in an attempt to limit the spread of the bacterial pathogen, Bordetella pertussis, to others. The inexorable whooping cough of pertussis is due to production of a cough inducing toxin elaborated by Bordetella. Unfortunately, once the toxin has been produced and the patient has symptoms, you are stuck. Stuck for six or more grueling weeks of cough. Annoying for adults, life threatening to infants. Better to vaccinate for pertussis and avoid getting it in the first place.

Cattle herd.
USDA.
Common domain.
5th: Vaccination creates herd immunity as a barrier to transmission of the infectious disease.
Now, in the case of measles the vaccine does prevent disease in the vaccinated (#1 above), to the tune of ~99% for someone who has received two vaccinations. And the vaccine also reduces the severity of illness in someone who still gets measles, despite vaccination (#2 above). The vaccine reduces complications (#3 above). And it reduces viral shedding and decreases secondary cases (#4 above). But measles vaccination also provides herd immunity, AKA ‘community immunity,’ in which the overall risk of measles transmission for everyone is reduced when a threshold percent of the entire population is vaccinated and immune.
Herd immunity only applies for certain infectious diseases: Ones in which there is no environmental reservoir (like surface water) and where there is either (1) no alternate host (such as wild animals) or (2) the alternate host can also be a target of prevention efforts. Measles is transmitted person-to-person. The virus can survive outside a human host for a few hours, but has no environmental reservoir. And it infects no alternate, non-human host which can serve as a reservoir of transmission. Other human pathogens that fit this bill for herd immunity include mumps, rubella, and smallpox. These can survive only by a continuous chain of transmission from one human host to the next. That’s pretty amazing when you think about it. The measles virus currently causing disease in a kid in California was spread by a continuous chain of human hosts reaching back 9- 10 centuries (when measles evolved from another virus, rinderpest, discussed in my previous post.)
So, if the virus needs to jump from one human host to the next in order to continue to survive, the obvious strategy to eliminate disease outbreaks (and potentially fully eradicate the disease) is to block that transmission. This creates a ring of immune hosts around any case of illness that occurs. When no secondary cases occur, voila, no outbreak. That’s herd immunity.
To better understand herd immunity, we have to talk mathematical modeling of infectious disease. Imagine a virus enters a nonimmune population – a group of people who have never previously been exposed to the infectious agent. In this setting, we can measure how many new cases originate from each case. This number is referred to as the “basic reproduction number” and is given the mathematical symbol R0.
R0 has been calculated for many pathogens in different outbreak settings. The number is not absolute: variables that impact R0 include the duration of infectivity of the sick and the number of susceptible potential hosts the sick come in contact with. For example, imagine a novel viral infection spread by droplets caused by coughing and sneezing as seen in this photo:

Sneeze.
CDC Public Health Image Library.
Common domain.
As a hypothetical example, let’s say the initial R0 of the virus is 6. This means for any case of infection, there are 6 secondary cases. If the mode of transmission of the illness is determined to be via droplet, public health authorities would encourage the public to use cough hygiene. The public might adopt wearing masks. The effect would be to reduce transmission. In Asia, where wearing masks during the flu season is socially accepted, the R0 of this fictional viral illness would be less than if the same viral illness appeared intially in the US. So I want to acknowledge that R0 is not a fixed number in all settings.
A significant implication of R0 is that if R0 is < 1, the outbreak will peter out. If R0 is > 1, the outbreak will continue to spread. The higher the R0, the greater the difficulty in containing the outbreak. The calculated R0 for Ebola for the west African outbreak was somewhere between 1.5 and 2.5. This helped reassure those fighting the outbreak that Ebola would not spread widely in the developed world where we have a vigorous public health infrastructure.
Another implication of R0 is that the higher the value of R0, the greater proportion of the population needs to be immune in order to prevent the chain of transmission to continue. This is referred to as the “herd immunity threshold” and is calculated:
1 – (1/R0)
To have adequate herd immunity in the population for a disease with an R0= 6 would require about 83% of the population to be immune. If the disease R0= 16, then 94% of the population would need to be immune.
If we are trying to get to the herd immunity threshold by vaccination, one also needs to take into account the efficacy of the vaccine. This is the proportion of vaccine recipients who develop immunity after vaccination. In the case of measles, the vaccine efficacy after one shot is about 94% and after two shots it is about 99%. What proportion of the population, then needs to be vaccinated with a partially effective vaccine to reach the herd immunity threshold? This is described as the critical vaccination level and can be calculated:
(1- (1/R0) / E
Where E = vaccine efficacy. So if you have a disease like measles, with a herd immunity threshold of 94% and a vaccine efficacy of 99% (after two shots), you need to have 95% of the population fully vaccinated to prevent outbreaks of disease. The efficacy is specific to each vaccine. As another example, mumps has an R0= 6 with a corresponding herd immunity threshold of ~83%. One would therefore think it would be much easier to prevent mumps outbreaks, but unfortunately the vaccine is not as effective as the vaccine for measles. After two doses of mumps vaccine, 88% of individuals have protective immunity. Thus you still need 94% of the population vaccinated to prevent outbreaks of mumps.
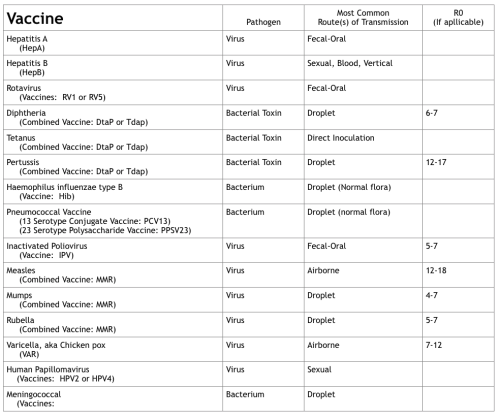
Here is a table of the routine recommended childhood vaccines:
And if all of the above is confusing, the Manchester Guardian has an interactive, computer model that illustrates the concept of herd immunity graphically.
Of course some people should not get vaccinated: vaccination is contraindicated in infants less than 12 months of age and immunocompromised patients. They must rely on the rest of us to get vaccinated for their protection (by herd immunity).
BONUS! 6th benefit: Vaccination reduces reliance on antibiotics to treat infections with resultant decreased antibiotic resistance.
Occasionally, vaccines have unexpected benefits. Reduction in antibiotic resistance in pneumococcal bacteria was one unexpected benefit associated with introduction of the 7-valent pneumococcal conjugate vaccine. The vaccine (also known by its trade name, Prevnar) was added to the recommended childhood vaccination schedule in 2000.
In the decade following the introduction of the vaccine, invasive pneumococcal disease rates fell in the target population. But more surprisingly, hospitalizations for pneumonia dropped, not only in the target population, but also in the elderly. The latter benefit is presumed to be due to a herd effect in which grandpa was not exposed to the grandchild’s pneumococcal pathogens.
Even more exciting was the observation that the rate of antibiotic resistant pneumococcal infections decreased. Antibiotic resistance is of increasing concern, because as pathogens become more resistant to antibiotics we are further limited in treatment options. Most ear infections in kids are viral and antibiotics are not needed. Providers are concerned, however, that they might miss the ear infection that isn’t due to a virus, but rather is due to pneumococcus which can cause severe complications. As a result, a significant number of unnecessary prescriptions for antibiotics are written for kids that had a viral ear infection. This is one driver of emerging pneumococcal antibiotic resistance. With the documented efficacy of pneumococcal vaccination in reducing the risk of ear infections.providders have written fewer prescriptions for these unnecessary antibiotics. The result has been improvement in the rate of resistance in pneumococcus.
In Conclusion:
Immunization has multiple benefits. Our ultimate goal is to improve the health of people. I get the notion that some patients want to limit their child’s exposure to medical risks and they think by avoiding or limiting vaccinations they may achieve that goal. Ironically though, they are increasing the child’s risk of receiving antibiotics, needing hospitalization, and suffering complications related to vaccine-preventable disease. The calculus is simple: the many benefits of vaccination outweigh the risks.
REFERENCES AND FURTHER READING:
Althaus, CL. 2014. Estimating the reproduction number of Zaire Ebolavirus (EBOV) during the 2014 outbreak in West Africa. PLOS Curr Outbreaks doi: 10.1371/currents.outbreaks.91afb5e0f279e7f29e7056095255b288. (Link)
Bellini, WJ, JS Rota, LE Lowe, et al. 2005. Subacute sclerosing panencephalitis: More cases of this fatal disease are prevented by measles immunization than previously recognized. J Infect Dis 192: 1686- 93. (Link)
Dagan, R, N Givon-Lavi, O Zamir, & D Fraser. 2003. Effect of a nonavalent conjugate vaccine on carriage of antibiotic-resistant Streptococcus pneumoniae in day-care centers. Pediatr Infect Dis J 22: 532- 40. (Link)
Fine, P, K Eames, & DL Heymann. 2011. “Herd immunity”: A rough guide. Clin Infect Dis 52(7): 911- 6. (Link)
Gastanaduy, P, A Cums, U Parashar, & B Lopman. 2013. Gastroenteritis hospitalizations in older children and adults in the United Sates before and after implementation of infant rotavirus vaccination. JAMA 310 (8): 851– 3.
Griffin, MR, Y Zhu, MR Moore, et al. 2013. U.S. Hospitalizations for Pneumonia after a Decade of Pneumococcal Vaccination. N Engl J Med 369 (2): 155- 63. (Link)
Musher, DM. 2006. Pneumococcal vaccine – Direct and indirect (“herd”) effects. N Engl J Med 354 (14): 1522- 4.
Orenstein, WA, RT Perry, & NA Halsey. 2004. The clinical significance of measles: A review. J Infect Dis 189 (Suppl 1): S4- S16. (Link)
Kyaw MH, R Lynfield R, W Schaffner, et al. 2006. Effect of introduction of the pneumococcal conjugate vaccine on drug-resistant Streptococcus pneumoniae. N Engl J Med 354 (14): 1455- 63. (Link)
Rodrigues, LC, VK Diwan, & JG Wheeler. 1993. Protective effect of BCG against tuberculous meningitis and miliary tuberculosis: A meta-analysis. Int J Epidemiol 22 (6): 1154–8. (Link)